 You should brush twice a day for two to three minutes at a time using a soft-bristled brush and fluoride toothpaste. 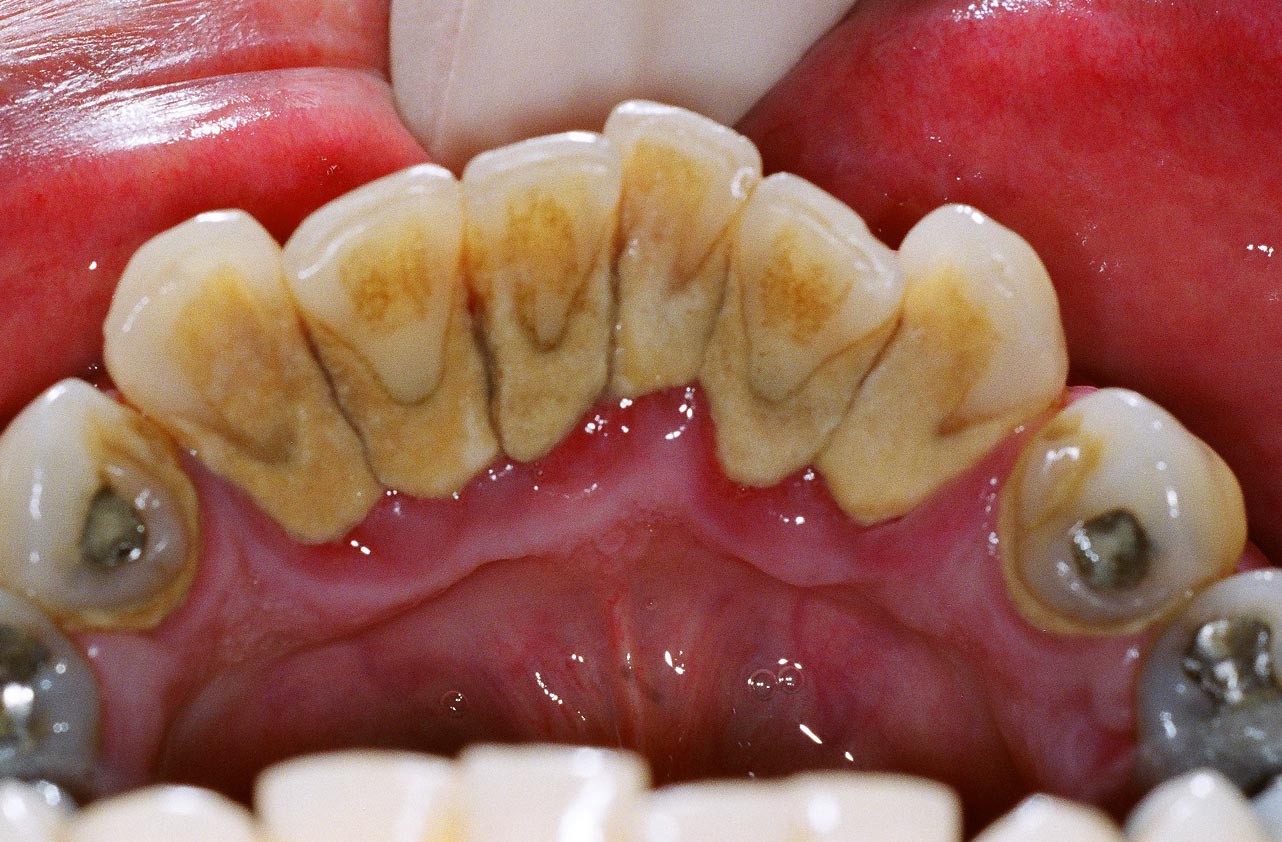 
Do that, as well as regularly visit with your dentist, and tartar will never be a problem. Plaque occurs before calculus, so the focus should be on removing and disturbing plaque on a daily basis. In some cases, oral surgery may be necessary in order to treat gum loss or bone loss that has occurred. Periodontitis usually requires your dentist to perform scaling and root planing. This allows the bacteria to attack not just the gum tissue but connective tissue and the supporting bone structures. Plaque continues to accumulate in these pockets and harden into tartar. The Mayo Clinic notes that pockets deeper than 4 millimeters are an indication of more advanced gum disease. Gums can recede prior to periodontitis but become a common symptom at this point. This generally happens because plaque has spread below the gumline, and tartar often helps this growth. Gingivitis will eventually progress to a more advanced stage of gum disease known as periodontitis. Gingivitis is reversible, and caught early enough, improved oral care at home may be the only treatment needed. Gingivitis can be rather silent in terms of symptoms, and when it does manifest symptoms, those include redness, swelling, and minor bleeding. The earliest stage of gum disease is gingivitis. Plaque causes periodontal disease, and this can occur before plaque has hardened into dental calculus. Subgingival Calculus and Periodontal Disease Your dentist will numb the tooth roots and gums to avoid any discomfort. Once found, your dentist will recommend cleaning it, which requires scraping using specialized dental tools. Often, patients are not even aware of subgingival calculus, and their dentists have to detect it using a dental explorer. This includes the cementum, which is weaker than even dentin, but also connective tissues and bone. Subgingival calculus not only affects your gums but aspects of your mouth below the gums. While supragingival calculus tends to be yellowish or whitish in color, subgingival calculus tends to be dark brown and even green or black. The difference is its position relative to the gumline. 
The Qualities of Subgingival CalculusĪs mentioned in the introduction, calculus can form above the gumline-supragingival-or below it-subgingival. That biofilm collects calcium, phosphorous and other minerals in the mouth, which is what causes the film to harden and to develop a much stronger adhesive bond. That plaque can accumulate anywhere in the mouth where it has access to nutrients, and bacteria on a shared surface form communities known as biofilm. Plaque forms as bacteria interacts with food particles and your saliva. Plaque can be removed by brushing and flossing, but tartar must be scraped away by a dental professional. When it calcifies, it bonds to those surfaces, not unlike how barnacles bond to boat hulls. Plaque is a sticky film that adheres to your teeth and other surfaces in your mouth. Subgingival calculus can result in gum disease and eventually tooth loss. Calculus can be either supragingival-above the gumline-or subgingival-below the gumline. Lacking good oral hygiene, plaque will not only build up but calcify into dental calculus, which is often called tartar. Plaque begins to form in your mouth whenever you eat, which is why diligent oral care is so important to oral health. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
